Cutting down cancer
Years of research collaboration produces successful therapies for brain cancer in dogs and lays foundation for human treatment
Years of research collaboration produces successful therapies for brain cancer in dogs and lays foundation for human treatment
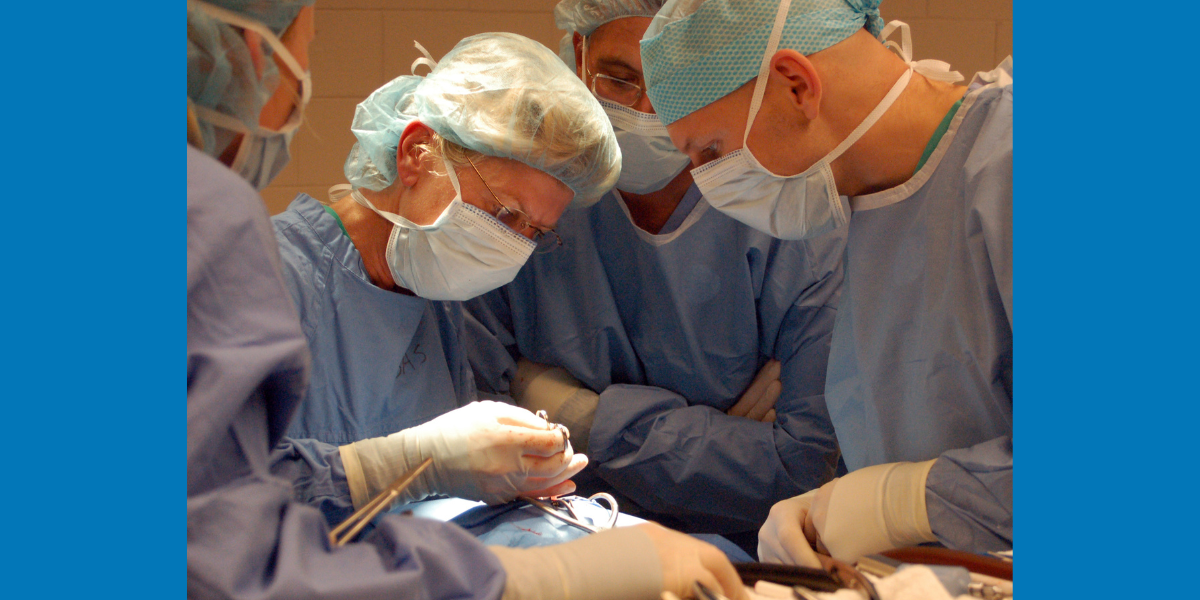
Dr. Liz Pluhar (left) performs surgery at the Veterinary Medical Center.
Batman, Otto, Alfie, and Huck have all shared the same title of canine cancer patient. They and other dogs enrolled in groundbreaking clinical trials at the University of Minnesota (UMN) College of Veterinary Medicine (CVM) also share another title: medical pioneers.
For 15 years, these dogs and others participating in the Canine Brain Tumor Clinical Trials Program have helped researchers deepen their understanding of glioblastoma—a type of brain cancer that is notoriously difficult to treat—and develop a targeted combination of immunotherapy and surgery that has improved the survival rates of patients that receive it.
To date, more than 400 dogs have been treated through the program, which is headed by Dr. Liz Pluhar, professor of surgery in the Department of Veterinary Clinical Sciences. Participating dogs with low-grade glioma and meningioma have responded well to the combination of surgery and immunotherapy, and dogs with high-grade glioma are seeing a prolonged disease-free interval while being provided an excellent quality of life. Grade refers to how aggressively or rapidly the cancer cells divide, with low-grade tumors growing more slowly than high-grade.
“When you treat somebody with a brain tumor with chemotherapy and radiation, it's like tossing an atom bomb into the patient—it goes off and kills everything,” Pluhar says. “Whereas, when you use immunotherapy, you train the body's immune system to recognize and attack only those tumor cells. It's a very directed approach, like using a guided missile just to kill the tumor cells. Because of that, there are many, many fewer side effects and in general, the patients feel fantastic. ”

The success of the program’s innovative therapies has been good news for not only canine patients but for human patients diagnosed with glioblastoma. Both species exhibit a similar immune response to tumors, and it’s that immune response that researchers have successfully manipulated in dogs to effectively kill cancer cells.
After achieving sustained success in canine trials, UMN researchers took the next step and announced in January 2021 that the first phase of a clinical trial to test the innovative treatment on human patients would begin enrolling. That milestone is the culmination of years of collaboration between CVM, the UMN Medical School, and the Masonic Cancer Center.
It’s also a testament to CVM’s long history of advancing veterinary medicine and is exemplary of its mission to transform new knowledge into better health for animals, humans, and the environment.
The opportunity to advance both veterinary and human treatment of glioblastoma is one that has taken shape over more than a decade of work by CVM and its partners.
High-grade gliomas, including glioblastoma, are one of the most commonly diagnosed primary brain cancers in dogs and carries a grim prognosis. The cancer’s tumors send off microscopic tendrils into the surrounding brain tissue, which are impossible to fully remove with surgery. Typically, dogs diagnosed with these tumors have few options and are often euthanized shortly after diagnosis.
The prognosis of a glioblastoma diagnosis isn’t much better in humans, who see a median survival of 14 to 16 months despite intense treatment. Glioblastomas account for more than 60 percent of brain tumors in adults, making the development of a treatment a priority for the medical community.
That’s where comparative oncology comes into play. It’s the study of using naturally developing cancers in animals as models for human disease. CVM researchers have long had people in mind while pioneering treatments for canine cancer.
Fifteen years ago this past August, Batman, a shepherd-mix whose black coloring and pointy ears earned him the name, was among those trailblazers. In 2008, Pluhar partnered with neurosurgeon, Dr. Stephen Haines, and successfully performed the first steps of an experimental procedure by removing his brain tumor and following up with an injection of gene therapy around the perimeter of the resection cavity. After the surgery, Batman received vaccine injections created from tumor tissue removed during his procedure. These injections caused Batman’s immune system to recognize any residual brain tumor cells and elicit a response.
One year later, a brain scan revealed no evidence of cancer and Batman received the all-clear. He later passed in 2010 from complications of an unrelated illness, but his story lives on in hundreds of dogs that also benefited from treatment with Dr. Matthew A. Hunt, now working with Pluhar to perform the brain surgeries.
“When I started doing this, the one thing that kept I kept hearing from people over and over again was that what I was doing gave them hope,” Pluhar says. “Over all the years we've been doing, giving somebody hope that there's something that we can do for their pet, and hopefully make them feel better and definitely extend their life with good quality of life has been very rewarding.”
Over time, the number of therapies and their combinations administered to dogs in the program has grown as new treatments have been developed. Vaccine-based immunotherapy and gene-based therapy remain part of the clinical trial but a breakthrough to improve the effectiveness of both therapies came at the hands of Michael Olin, PhD., associate professor, and Dr. Christopher Moertel, professor, both in the Department of Pediatrics at the UMN Medical School.

While the vaccine and gene-based approaches were successful at extending most of the canine patients’ survival, the tumors always recurred. Olin discovered a protein, known as CD200, was blocking the body’s natural immune response to the cancer. Tumor cells express the protein on their surface and shed it as well, and an inhibitory receptor for CD200 is found on the surface of immune cells. When CD200 binds to the receptor, an “off” signal is sent to the immune cells and prevents them from activating to help kill cancer cells.
Olin manufactured peptides that would override the tumor’s efforts to protect itself from the body’s immune response. The increased effectiveness of the enhanced therapy in canine trials has doubled survival times in the dogs treated and served as the foundation for the launch of the latest round of human clinical trials at the UMN. Previous human clinical trials have focused on treating patients with earlier versions of the gene and immunotherapy therapies.
“The opportunity to actually see the work that we did in dogs being translated to human patients, meeting some of the human patients that had received the therapy, and hearing the stories that they would tell about how much better they felt when they were getting immunotherapy has been incredible,” Pluhar says.
The success of the glioblastoma clinical trials and research at the UMN is helping shine the spotlight on the importance of comparative oncology and the healthier future it could unlock for dogs and humans alike.
That includes taking steps to take UMN’s innovative cancer treatment from the lab to veterinary clinics around the United States.
Earlier this year, the research team completed a license agreement with a veterinary biotechnology company, Ardent Animal Health, to distribute the treatment. Ardent Animal Health develops novel biological treatments for aging-related and inflammatory diseases including cancer. The licensing agreement provides a path to affordable and broadly applicable cancer treatment for dogs at veterinary clinics across the U.S.

On the human health side, another biotechnology company that produces Olin’s peptide to treat human GBM patients, OX2 Therapeutics, is working to bring the glioblastoma treatment to people and is sponsoring the UMN human clinical study.
The impact of this treatment isn’t limited to glioblastoma. Researchers believe it could be tailored to a number of other cancer types, including melanoma, breast cancer, and bladder cancer. It’s welcome news as cancer remains the second leading cause of death for adults in the United States, according to the Centers for Disease Control and Prevention.
In 2022, the American Cancer Society estimated that 1.9 million people were diagnosed with cancer and another 600,000 died as a result of the disease. The numbers paint a stark reality and underline the need for treatments like those developed at UMN.
That need is driving a host of support for UMN’s research. Many people and organizations have contributed funding to keep research progressing over the years, including Humor to Fight the Tumor, the Randy Shaver Cancer Research and Community Fund, the American Brain Tumor Association, the American Kennel Club, the American Cancer Society, the National Cancer Institute at the NIH, Bob and Corrine Ferris, Shepherd Trust Fund, the Dahlberg Family Foundation, Love Your Melon, Children’s Cancer Research Fund and Hyundai Hope on Wheels.
The collaboration across UMN, private industry, and philanthropists is vital to continue the advancement of cancer treatments and bring both humans and animals a step closer to healthier, longer lives.
“It's been very rewarding being here and being able to closely interact and be very close colleagues across campus. We work with neurosurgeons, neurooncologists, and researchers in the laboratories on a regular basis,” Pluhar says. “If we weren't all working together as a team, we wouldn't be able to do what we're doing here. We each have our areas of expertise that we bring to the process, and I think that’s what makes us unique and successful.”
The 2022-2023 school year marks the 75th anniversary of the University of Minnesota College of Veterinary Medicine.
Join us as we revisit milestones and innovations in the College's history and look forward to our future success in advancing veterinary medicine through teaching, research, and service.